Demographic Disparities in Vaccination Rates
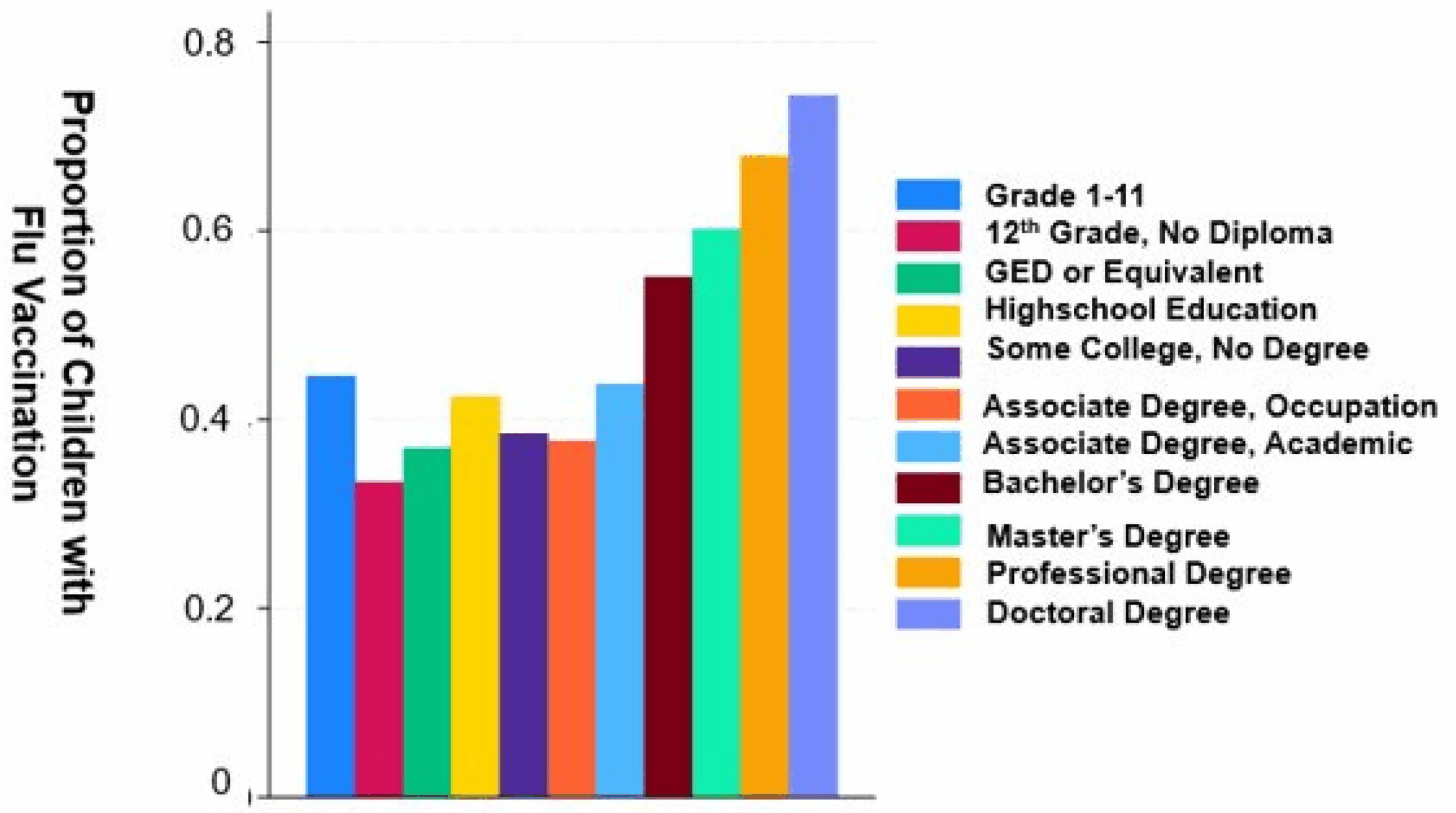
Racial and ethnic disparities in flu vaccination coverage have persisted and, in some cases, widened. In the 2021–2022 season, around 54% of White and Asian adults received the flu shot, compared to just 42% of Black adults, 38% of Hispanic adults, and 41% of American Indian/Alaska Native adults. Although there were modest gains for Black and Hispanic populations in subsequent seasons, these groups still lagged behind White adults by several percentage points. By 2023–24, Black adults trailed by about eight percentage points, Hispanic adults by eleven, and American Indian/Alaska Native adults by fourteen.
Geography and socioeconomic status also played significant roles. Adults living in rural areas had lower flu vaccination rates—about 40%—compared to 48% in urban and suburban communities. Access to healthcare, trust in medical institutions, and convenience were all contributing factors.
Reasons for the Decline
1. Pandemic Disruptions
The COVID-19 pandemic disrupted routine medical visits, which are typically when adults receive flu shots. Lockdowns, fears of exposure, and overloaded healthcare systems shifted priorities away from seasonal flu prevention. Many patients skipped preventive care entirely, while providers focused more on COVID vaccination and testing.
2. Vaccine Fatigue and Misinformation
As COVID-19 vaccination campaigns intensified, many Americans began to experience what experts called “vaccine fatigue.” The continuous stream of vaccine-related news, appointments, and recommendations overwhelmed some individuals, making them less likely to pursue additional vaccinations such as the flu shot. Simultaneously, widespread misinformation about vaccines—amplified online and through social media—undermined public trust in all vaccines, including the influenza vaccine.
A 2024 survey showed that while 67% of adults agreed that flu shots prevent serious illness and hospitalization, only 38% stated they definitely planned to receive the flu vaccine in the upcoming season. Nearly half of respondents said they were unsure or had no intention of getting vaccinated.
3. Social Determinants of Health
Structural barriers continued to influence vaccination rates. Factors such as income inequality, lack of reliable transportation, limited time off work, and low health literacy disproportionately affected low-income and minority communities. Even among those with health insurance, these social determinants of health created significant obstacles to consistent vaccine uptake.
Public Health Implications
Tramadol should be used with caution in individuals with:
Liver or kidney disease
Epilepsy or seizure disorders
A history of mental illness or addiction
Breathing problems such as asthma or COPD
It can interact with various medications, including sedatives, antidepressants, antipsychotics, and other opioids. Combining tramadol with alcohol or benzodiazepines significantly increases the risk of respiratory depression and death.
Moving Forward
To reverse this trend, public health officials are calling for renewed outreach strategies. These include bundling flu and COVID-19 shots, increasing access through pharmacies and walk-in clinics, and launching community-based education campaigns. There is also a push for healthcare providers to make strong, consistent recommendations for flu vaccination during routine visits.
Addressing vaccine hesitancy, combating misinformation, and dismantling access barriers are critical steps toward increasing coverage. Ensuring that flu vaccination remains a trusted, accessible, and routine part of adult healthcare will be vital in protecting public health in future seasons.