Introduction
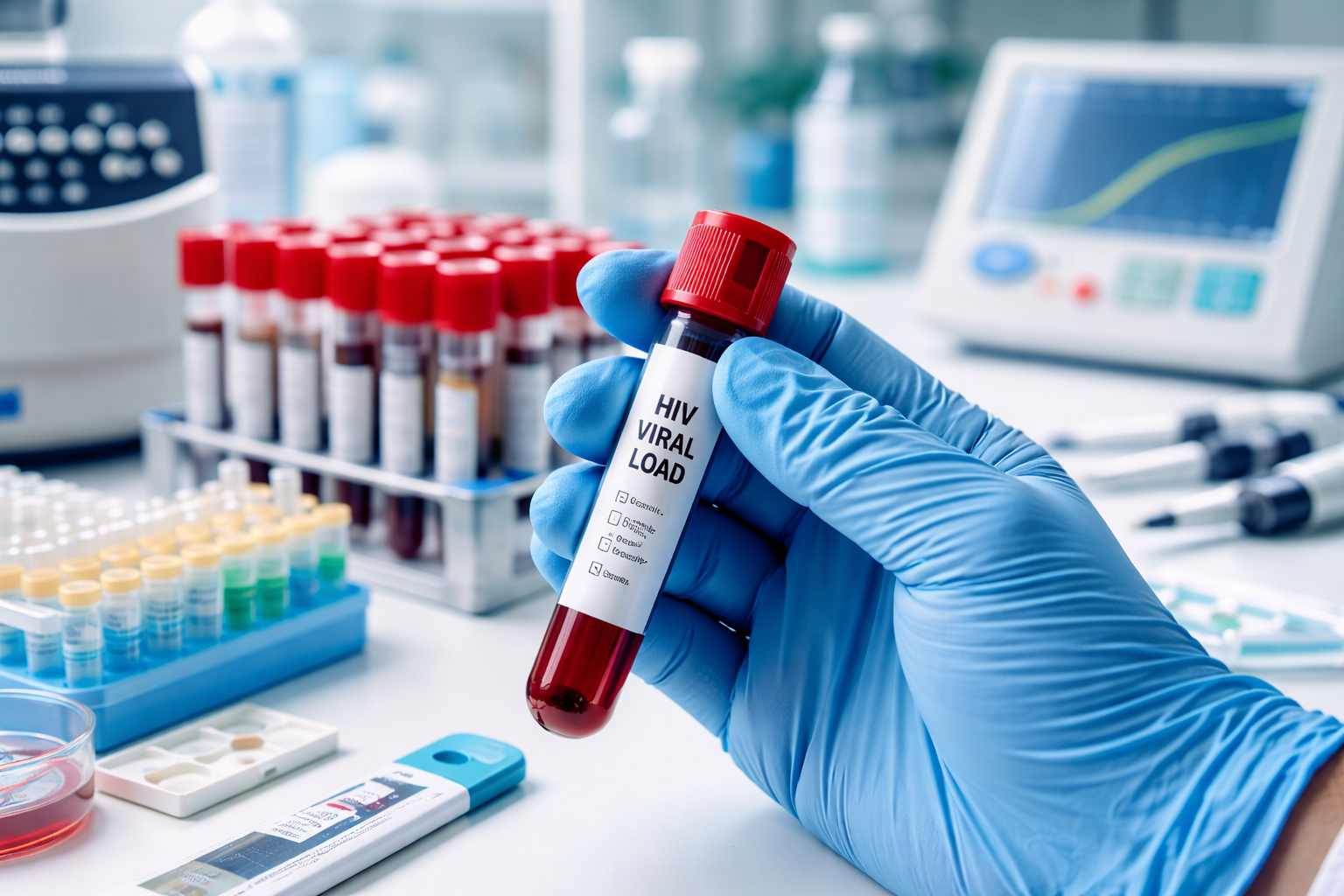
Human Immunodeficiency Virus (HIV) remains a major global public health concern. Early diagnosis and immediate linkage to care are crucial for improving patient outcomes, preventing disease progression, and reducing transmission. One promising advancement in HIV management is the availability of HIV viral load testing with next-day results, which provides rapid information about the amount of virus in a patient’s blood. Although faster results are expected to motivate patients to engage in care quickly, research indicates that next-day viral load testing alone does not significantly improve linkage to care. This finding highlights the complexity of healthcare engagement and the multiple factors influencing patient behavior.
Importance of HIV Viral Load Testing
Viral load testing is a key component of HIV management. It measures the number of copies of HIV in the bloodstream and helps determine disease stage, treatment effectiveness, and risk of transmission. Traditionally, viral load results may take several days or weeks to return. Delays can lead to patient anxiety, missed follow-up appointments, and treatment postponement. Therefore, next-day viral load testing has been introduced to accelerate clinical decision-making and improve patient experience.
Concept of Linkage to Care
Linkage to care refers to the process of connecting individuals diagnosed with HIV to medical treatment and support services. This includes attending the first clinical appointment, starting antiretroviral therapy (ART), and receiving ongoing medical monitoring. Successful linkage is essential for viral suppression, improved immune function, and long-term health. Despite technological improvements in testing, many individuals face barriers such as stigma, transportation challenges, lack of social support, fear of disclosure, and financial constraints that influence whether they remain engaged in care.
Next-Day Results and Patient Behavior
Providing next-day viral load results was expected to encourage patients to return promptly for follow-up visits and begin treatment sooner. However, studies show that rapid availability of results does not significantly change rates of linkage to care. While patients appreciate faster information, the decision to engage in care is shaped by emotional readiness, personal beliefs, socioeconomic conditions, and healthcare system factors. Simply shortening the waiting period for test results does not overcome these deeper barriers.
Healthcare System Factors
Healthcare infrastructure plays a major role in patient engagement. Long waiting times at clinics, complicated appointment systems, limited clinic hours, and lack of culturally sensitive care can discourage patients from returning. Even with next-day results, individuals may struggle to navigate the healthcare system. Without additional patient support such as counseling, navigation services, and follow-up reminders, faster test results alone are insufficient to ensure continuity of care.
Psychological and Social Influences
An HIV diagnosis often triggers fear, anxiety, denial, and social stigma. Some individuals may avoid care due to fear of discrimination or disclosure to family and community members. Others may struggle with mental health challenges such as depression and substance use, which interfere with consistent medical engagement. These psychosocial factors strongly influence whether patients link to care, regardless of how quickly laboratory results are available.
Conclusion
Although next-day HIV viral load testing enhances clinical efficiency and patient satisfaction, it does not independently improve linkage to care. Effective HIV management requires addressing psychological, social, and systemic barriers alongside technological advancements. A holistic healthcare approach that prioritizes patient support and engagement remains essential for ensuring timely treatment initiation and long-term viral suppression.